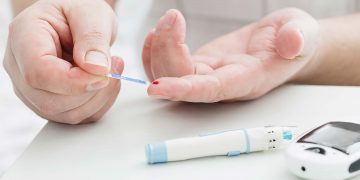
Diabetes insipidus (DI) is a condition with some of the same early signs as diabetes mellitus. The main early signs of diabetes insipidus are excessive thirst and frequent urination. The urine tends to be pale or sometime almost the colour of plain water. This pale colour is because the urine is severely diluted. The fluid intake has nothing to do with the frequent urination. The excessive thirst is just a way for the body to replace some of the lost fluids.
There are several different types of Diabetes Insipidus and each with a different cause:
The most common type is neurogenic DI – this caused by a deficiency of arginine vasopressin (AVP), also known as antidiuretic hormone (ADH).
The second common type of DI is nephrogenic diabetes insipidus, which is caused by an insensitivity of the kidneys to ADH. This damage can also be as a result of an iatrogenic artifact . The terms iatrogenesis and iatrogenic artifact refer to inadvertent adverse complications caused by or resulting from medical treatment or drug use.
Signs and symptoms of diabetes insipidus
- The main symptoms of this type of diabetes are Excessive urination and extreme thirst. The Symptoms of diabetes insipidus are quite similar to those of untreated diabetes mellitus. However the main distinction is that the urine is not sweet as in diabetes mellitus – it does not contain any glucose.
- There is also not hypoglycemia or hyperglycemia as it does not cause an elevation in blood glucose levels.
- You will probably have no blurry vision. If it does occur is a rarity.
- Signs of dehydration may also appear in some individuals since the body cannot conserve much (if any) of the water being drank.
- The extreme urination normally continues throughout the day and the night – like a real siphon.
How does diabetes insipidus affect children?
In children, DI can interfere with appetite, eating, weight gain, and growth as well.
DI may present itself with fever, vomiting, or diarrhea.
How will it affect my health?
You can live with untreated DI and remain healthy for decades. The only requirement is that you drink more water than what you lose to offset the loss through urination. There is however a real risk of dehydration and loss of potassium.
How to distinguish diabetes mellitus from diabetes insipidus
In order to distinguish DI from other causes of excess urination, blood glucose levels, bicarbonate levels, and calcium levels need to be tested.
Measurement of blood electrolytes can reveal a high sodium level (hypernatremia as dehydration develops). Urinalysis demonstrates dilute urine with a low specific gravity. Urine osmolarity and electrolyte levels are typically low.
Fluid deprivation tests helps determine what the causes are of do DI whether it is by:
- excessive intake of fluid
- a defect in ADH production
- a defect in the kidneys’ response to ADH
This test measures changes in body weight, urine output, and urine composition when fluids are withheld and as dehydration occurs.
The body’s normal response to dehydration is to concentrate urine and conserve water, so urine becomes more concentrated and urination becomes less frequent.
People with DI continue will tend to pass large amount of dilute urine in spite of not drinking any fluids. Sometimes measuring blood levels of ADH during this test is also necessary.
How to distinguish between the main forms of DI
- To distinguish between the main forms, desmopressin stimulation is also used; desmopressin can be taken by injection, a nasal spray, or a tablet.
- While taking desmopressin, you should drink fluids or water only when thirsty and not at other times, as this can lead to sudden fluid accumulation in the central nervous system.
- If desmopressin reduces urine output and increases osmolarity, the pituitary production of ADH is deficient, and the kidney responds normally.
- If the DI is due to renal pathology, desmopressin does not change either urine output or osmolarity.
- If central DI is suspected, testing of other hormones of the pituitary, as well as magnetic resonance imaging (MRI), is necessary to discover if a disease process (such as a prolactinoma, or histiocytosis, syphilis, tuberculosis or other tumor or granuloma) is affecting pituitary function.
- Most people with this form have either experienced past head trauma or have stopped ADH production for an unknown reason.
- Habit drinking (in its severest form termed psychogenic polydipsia) is the most common imitator of diabetes insipidus at all ages.
- While many adult cases in the medical literature are associated with mental disorders, most people with habitual polydipsia have no other detectable disease.
- The distinction is made during the water deprivation test, as some degree of urinary concentration above isosmolar is usually obtained before the patient becomes dehydrated.
There are several forms of DI:
- Neurogenic
- Nephrogenic
- Dipsogenic – is due to a defect or damage to the thirst mechanism, which is located in the hypothalamus. This defect results in an abnormal increase in thirst and fluid intake that suppresses ADH secretion and increases urine output.
- Gestational – occurs during pregnancy. While all pregnant women produce vasopressinase in the placenta, which breaks down ADH, this can assume extreme forms in GDI. Diabetes insipidus is also associated with some serious diseases of pregnancy. These are pre-eclampsia, HELLP Syndrome and Acute fatty liver of pregnancy.
Treatment of DI
People with DI need to be properly hydrated as they may become dehydrated very easily.
Treatment with drugs
Central DI and gestational DI respond to desmopressin. Carbamazepine, an anti-convulsive medication, has also had some success in this type of DI.
Gestational DI tends to become less active or die down on its own 4 to 6 weeks after labour.
Some women may develop the condition again in subsequent pregnancies. Most cases of gestational DI can be treated with desmopressin. In rare cases, however, an abnormality in the thirst mechanism causes gestational DI, and desmopressin should not be used.
Desmopressin will be ineffective in nephrogenic DI. Instead, the diuretic hydrochlorothiazide (a thiazide diuretic) or indomethacin can improve nephrogenic diabetes insipidus.
Thiazide diuretics are sometimes combined with amiloride to prevent hypokalemia.
Lithium-induced nephrogenic DI may be effectively managed with the administration of amiloride, a potassium-sparing diuretic often used in conjunction with thiazide or loop diuretics.
Thiazide diuretics have been administered for lithium-induced polyuria and nephrogenic diabetes insipidus.
However, recently amiloride has been shown to be a successful treatment for this condition.
more info could be obtained from:
- The DiabetesInsipidus Foundation, Inc
- Information on DiabetesInsipidus